HRC image
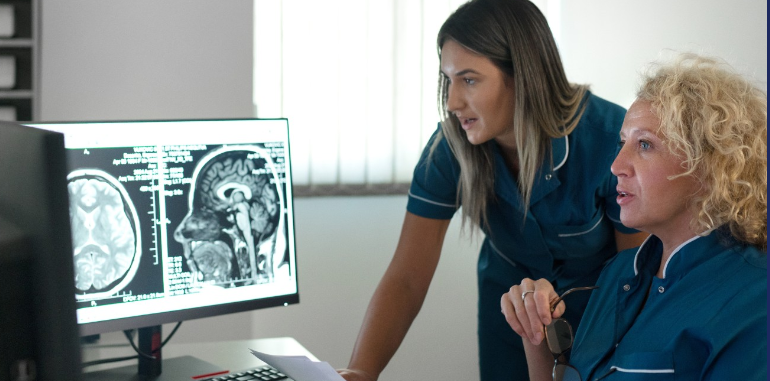
The HRC in Brain injury supports researchers and innovators to identify unmet needs, evaluate the effectiveness of their technology and implement these solutions to improve the quality of life of those affected by brain injury. Acute care, monitoring of neurological disorders, physical and psychological rehabilitation techniques, and regenerative medicines can all reduce long-term injury and improve long term health. The team works closely with its network of national partners, to support research at every stage of development. They work with patients, carers, and families, to ensure that innovation is meeting a need within the community and making a real difference to those who need it most.
About HRC's theme
Conditions affecting the brain and spine affect large numbers of people and often have a significant impact on their quality of life. Brain injuries can be overwhelming for people, their families, and society. Brain development at the beginning of life (e.g., prematurity, acquired brain injury), and brain degeneration at the end of life (e.g., frailty, co-morbidities) are both areas where specialised care is required. Long-term acquired brain injuries (or ABIs) are also common in people who have had sports concussions, falls or head injuries as a young child, and the homeless and prison population frequently report a history of brain injury.
Support provided
- Reduce Acquired Brain Injury (ABI) by focusing on the three forms of injury prevention: primary prevention – increase the knowledge of the causes of ABI and educate communities working with at-risk groups on how to prevent ABI; secondary prevention – improve screening and diagnosis of ABI to increase early intervention and reduce long-term brain injury; and tertiary prevention – improve the ability to identify individuals experiencing ABI in the community and improve access to care services for those with brain injury.
- Improve acute care in hospitals and monitoring brain activity following this, to improve recovery pathways for those with brain injury. In particular: improving imaging used for diagnosing mild and severe TBI (traumatic brain injury), including using AI to analyse CT scans in emergency departments; neuroprotective innovations to reduce secondary brain injury acquired during recovery; multimodality monitoring of brain injury, using biological markers to track recovery; supporting surgical innovations to improve technologies used during neurosurgery; and reporting neurological outcomes when assessing other areas to raise awareness across services to improve brain care.
- Use new neuro-imaging, innovative approaches for assessing intracranial dynamics, and the application of molecular testing of brain tumours. In particular: the evaluation of PET markers and the clinical application of el imaging approaches including MRI scan data for tumour treatment planning, leading to safe and improved resection of tumours; molecular diagnostics, including whole genome analysis of tumour tissue for improved diagnostic classification, and analysis of cell-free DNA for early diagnosis and monitoring; improving non-invasive intracranial pressure monitoring by improving models for estimation and applying machine learning techniques to monitor this; and evaluation of dynamic imaging to evaluate CSF disorders, including PC-MRI application in normal pressure hydrocephalus, and determination of physiological brain compliance.
- Support bespoke rehabilitation interventions, targeted cognitive assessments, and frameworks for systematic evaluation; utilisation of human cellular models of disease; evaluation of neuroprotective agents, surgical approaches, and targeted therapies.
- Understanding brain health at the beginning and end of life. For neonatal care, this includes: improving pathways and evaluation of the importance of baby-parent contact; new technology in neonatal brain imaging, including the development of the fUSiON project cot-side functional brain imaging device for intensive care; expansion of the genomic screening for the diagnosis of rare childhood diseases. For elderly medicine, this includes: improving recognition, treatment and ongoing care of under-diagnosed, treatable conditions in the elderly (such as cervical myelopathy and idiopathic normal pressure hydrocephalus); reducing the need for elderly people to visit hospital by developing community alternatives to delivering neurological rehabilitation (such as telerehabilitation, providing these to homes and local care facilities).
- Prevention and education
- Acute care monitoring
- Restoration and rehabilitation
- Diagnostics
- Life course
- Digital, AI and data
- Neurosurgery registries (secure data environment and hosting for registry information

